Since about a month ago, the coronavirus infection and death rates spiked in the country. While the infection rate was 10 per cent before, it rose to 50 per cent and the daily death toll tripled. The spikes came as a reality check for the public health experts.
Following the two signs of the crisis, the local administration issued a prohibitory order in Kathmandu valley and the Ministry of Health issued a circular to all hospitals across the country to provide treatment to Covid-19 patients. And, the National Trauma Centre was one of them.
To address the health crisis, the centre’s director Dr Santosh Poudel discussed with the hospital team whether or not to treat the Covid-19 patients. In the past, the centre was involved in the treatment of people injured in various accidents.

He got a positive response and began the service. One month on, the centre has proved efficient in emergency medical management and preparedness that many other hospitals in the country can learn from.
Problems
However, there was a problem to relocate the injured patients being treated there, some in line to get an operation, others in OPD wards.
Meanwhile, the MoHP directed converting Bir Hospital’s new surgical building into the Covid-19 unified hospital and move the trauma patients to the older Bir Hospital. The patients in need of operation were shifted to Orthopaedic Hospital in Jorpati.

Encouraged by the ministry’s decision, Dr Poudel also expressed commitment to treat the infected. And, starting May 9, the trauma centre started treatment of Covid-19 patients.
Poudel shares that the initial days, however, were too troubling. According to him, 177 patients were admitted on the first day and many others were sent back due to a lack of beds. But soon after, the stock of liquid oxygen ran out at the centre.
And then, more than a dozen hospitals across the country issued statements saying they are unable to provide treatment due to the lack of oxygen.

The trauma centre was getting its oxygen from the Shankar Oxygen Gas Industry in Balaju. But, it had been affected by the quota system of the Covid-19 Crisis Management Centre (CCMC).
With increasing pressure, the centre needed 450 oxygen cylinders daily. The oxygen company had limited its supply as per the CCMC’s instructions and informed the hospital that it can give only 50 cylinders.
Hence, the hospital patients did not get oxygen even after running around the city. In this situation, Director Poudel shares that the team was afraid of being liable to a crime of backing out from the commitment it made to treat the infected.
“Even after getting oxygen delivered in ambulances all night, it would last only till 7 in the morning,” he shares. He even took it to social media the same day, saying, “Now, because oxygen cannot be provided immediately, 105 patients are at the mercy of the god.”
He says he had sought help on social media as he did not want to be left with regrets. “I couldn’t sleep because of fear that more than 100 patients would be displaced due to lack of oxygen supply on time.”
Solutions

Currently, 125 beds at the trauma centre are occupied by Covid-19 patients. Of these, 80 beds are under the High-Dependency Unit (HDU) and 35 beds under the emergency ward where eight beds have ventilators. Similarly, there are 10 beds in the Intensive Care Unit (ICU) beds.
After the hospital started running out of oxygen, Dr Poudel inquired the company about it in an evening. The supplier replied, “The police have taken it away!” After receiving such an irresponsible response, Poudel started looking elsewhere, all night, to solve the problem and even lodged a complaint at the Ministry of Home Affairs.
The next morning, when the liquid oxygen arrived, the oxygen crisis was pushed back for five days.
Poudel says because the hospital beds already had oxygen ports and connections to oxygen liquid tanks, he had felt confident enough to start the treatment of Covid-19 patients. He says he dared so while risking his career would end if anyone died due to the lack of oxygen.

—
While experts were warning that a second wave could strike at any time and cause major damage, the trauma centre was training health and sanitation workers in the treatment and management of Covid-19 patients and mentally prepared them for the chaos ahead. Poudel says he realised early that the centre could not stay on the sidelines during the epidemic, else the nation would suffer a big loss. “Emergency preparedness is not practised in Nepal, but we did it.”
According to Poudel, even though the HDU beds are empty now, the problem regarding beds with oxygen and ventilator is the same. He says it is still resulting in the deaths of the patients.
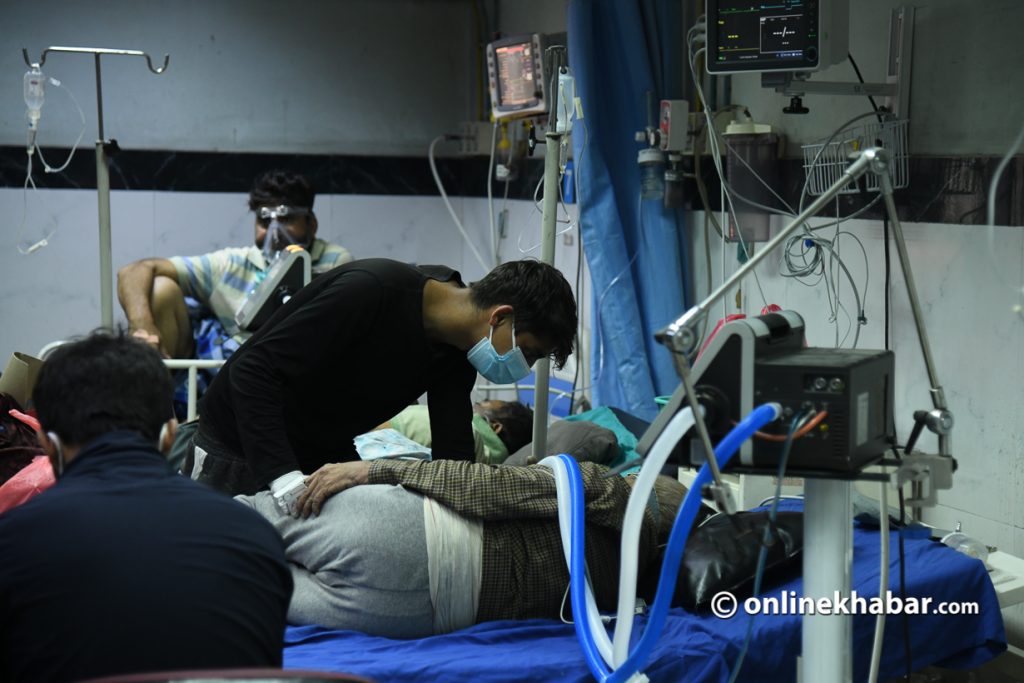
But, the treatment of coronavirus patients is still stressful. Health workers are rattled to hear the cries of death and infection every day. “We have arranged isolation for our health workers in hotels so that the stress of infection does not reach their families. Whereas the hospital has also arranged food for the infected,” he informs claiming the hospital is providing facilities in its own capacity.
Although the centre started the operation in a short time, he claims it has not sent anyone coming there seeking treatment empty-handed. “For the first week, we worked very hard. The pressure decreased day-by-day after that,” he claims.
According to him, the hospital is providing its services by using the ICU wards when the emergency gets full. “To have 18 ICU beds at a hospital that treats injuries is a big deal. And, since there’s no situation to set up new ICU beds right now, our resources have been useful.”
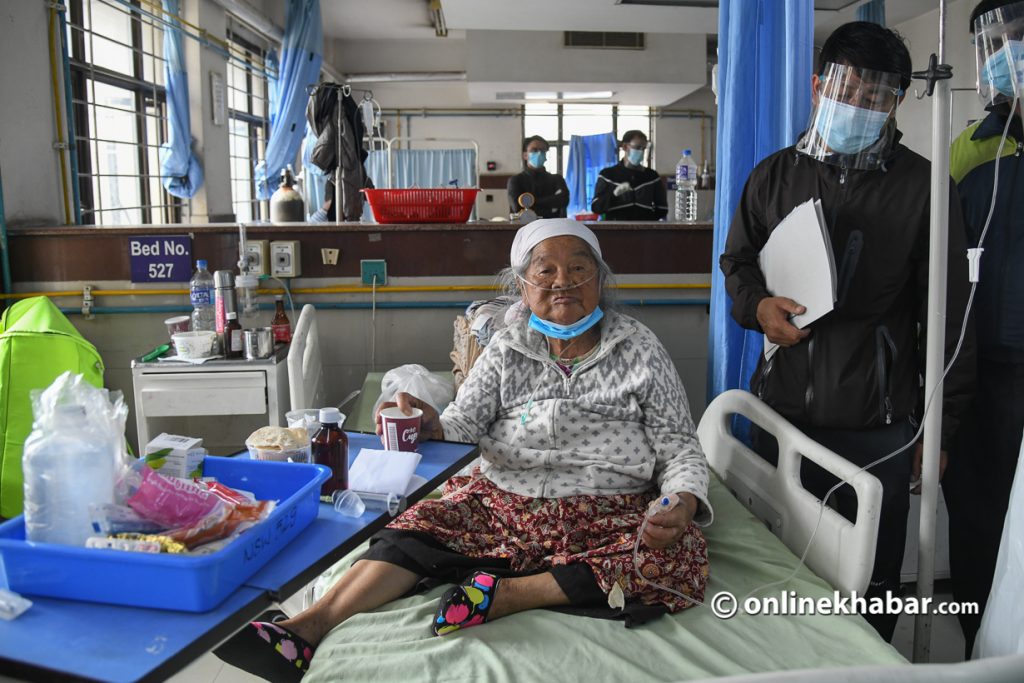
Meanwhile, he expresses that he is happy with the contribution made by the government health institutions during the crisis. Tribhuvan University Teaching Hospital, Patan Hospital and APF Hospital have a large number of infected people, and their contributions have been incomparable.
But, he stresses that the pandemic has taught all hospitals the importance of emergency preparedness. And, that everyone should understand that the government will fail in the crisis if the health institutions are not efficient.