To reach the point to make tuberculosis preventable and curable, Nepal took decades. Yet even after six decades of work and with the success seen in the awareness of the disease, Nepal is still struggling to eliminate it completely. The situation is concerning as almost half the population are infected with tuberculosis in Nepal whereas it is in the top 10 causes of death.
The National Tuberculosis Control Center (NTCC) at Madhyapur Thimi came into existence in 1989 and since then has organised and overseen many nationwide programmes to detect, treat and cure tuberculosis as well as conducted various awareness programmes. Its new Director Sanjay Kumar Thakur took over the leadership role just about a month ago but has more than 25 years of experience working in the remotest parts of Nepal, from the time when the disease was shrouded in stereotypes.
In an interview with Onlinekhbar, on the occasion of World Tuberculosis Day, Dr Thakur says there is much to do at the community level regarding the end and elimination of tuberculosis in Nepal.
Excerpts.
What is the recent status of tuberculosis in Nepal?
If we look at the nature of tuberculosis as a disease, it has changed a lot from the past. But, its tendency has not changed much in the last few years. In the case of Nepal, we record about 69,000 new cases every year with 191 new cases every day. It has an estimated 16,000 deaths every year with 44 deaths every day.
Of the total patients suffering from tuberculosis in Nepal, 67 per cent are male and 33 per cent are female. Given the recent data, the senior citizens or the older population are seen to be more infected whereas 6.6 per cent of the infected are from the 0-14 age group with a 5 per cent increase rate in adolescents from the previous year.
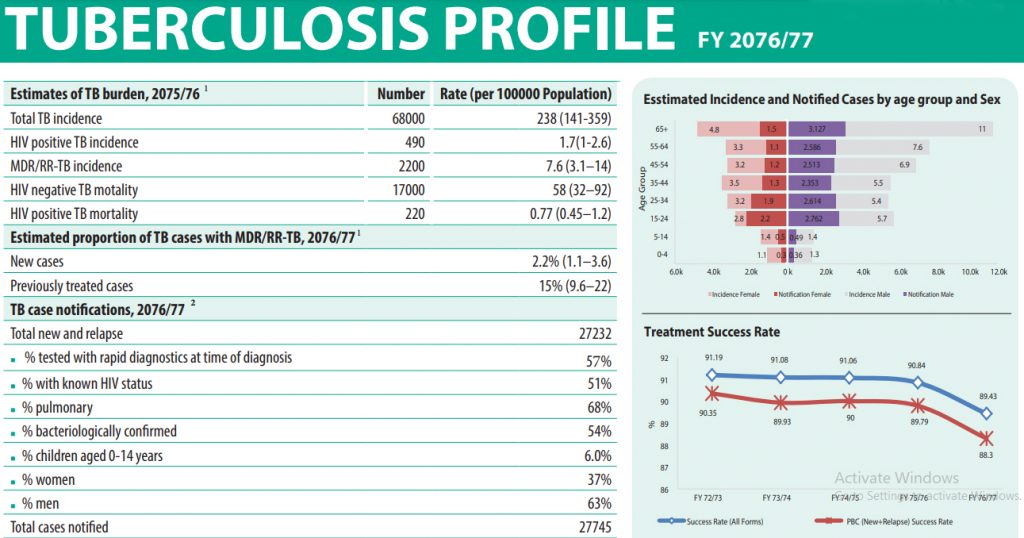
But recently, Nepal was listed as one among the top 30 high (multidrug/rifampicin-resistant) MDR/RR-TB burden countries by the World Health Organization for 2021-2025 and this is a concerning issue.
So what is your centre’s next course of action?
We have drafted a new five-year action plan for 2021-26. It has been approved and we will soon go into implementation. The plan aligns with Nepal’s pledge to end tuberculosis by 2035 and eliminate it by 2050.
This year’s theme of World TB Day is ‘Invest to End TB:Save Lives’ and following our action plan, we aim to build the necessary infrastructure, mobilise human resources, set up and increase access to diagnostic tools, tests and drugs. For this, we need both economical and cooperative investment from all three tiers of governments as well as the health institutions along with supporters like the WHO and Save the Children among others. The three tiers of government have given their commitment already.
With the action plan, we also plan to increase the fund investment by 70 per cent to minimise the gaps and overlaps. The Global Fund through Save the Children is investing in the programme and we hope to better the odds. We have already moved forward with the TB-free municipality programme in 30 local units and for the next five years, we aim to reach all of them. For this, we are also shifting from the centre-to-bottom approach to the bottom-to-top approach, to strengthen the local level for the programme to be most effective.
Neary 70,000 new tuberculosis cases per year is not a small number and it is also one of the top reasons for death. Despite its seriousness, why have we not curbed the infection yet?
There are more than 100,000 active tuberculosis cases every year. There are over 5,000 DOTS centres and with the intake of regular and right drugs, the infection can be stopped from spreading within a few weeks.
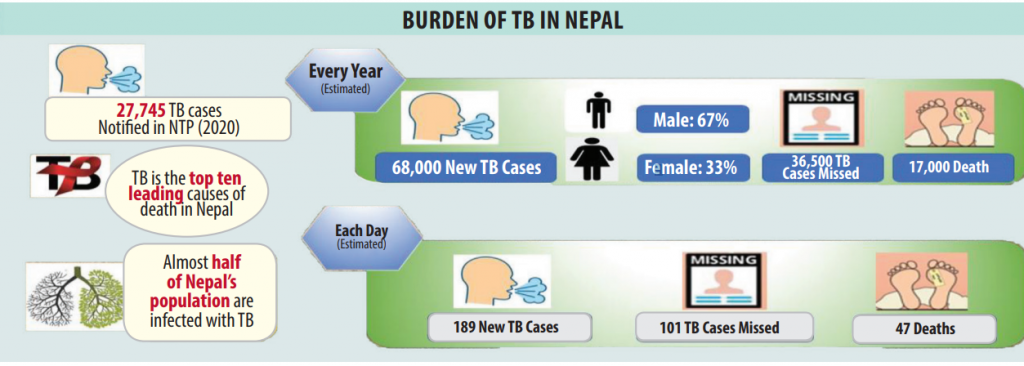
But, in our recent preliminary survey, we found that only 50 per cent of the infected have enrolled themselves in the National Tuberculosis Programme. The incubation period of tuberculosis is between two to 12 weeks, during which a patient, after being symptomatic, can also transmit the infection to others. But, in Nepal, especially outside the urban areas, there is a lack of knowledge regarding the presumptive cases and problems with early identification.
Nepal is still suffering from malnutrition which subsequently compromises people’s immunity, one of the factors in one contracting TB. Likewise, there are people who suffer from co-infection including HIV and diabetes while they continue to live in closed settings with poor ventilation.
On the one hand, people avoid early checkups and, on the other, those infected do not follow the drug therapy properly and regularly during the six to 12-month course. Then, there is another factor: the lack of prescription of a combination of drugs and the increasing drug resistance seen in the patients.
Also, access to testing is low and contract tracing is poor. Diagnostic facilities are yet to reach everywhere, only 62 out of 77 districts. Gene-Xpert tests are expensive and microscopic tests are not enough to determine the symptoms. So the infection within the community and family members have been difficult to control.
Other than that, problems arose following weak network problems where individuals were not working together. Also, when the country went into federalism, the human resources we had was redistributed and then the priority shifted. The upcoming elections will impact the programme too as they will create a gap in the leadership in the local units. But, the five-year programme will continue and be implemented after the elections.
So does that mean that the drug for tuberculosis is not working?
No, treatment for tuberculosis is effective with one or multidrug therapy. The DSTB treatment success rate is 91 per cent with a death rate of 3.3 per cent whereas the DR TB treatment success rate is 71 per cent with a death rate of 13 per cent.
But, drug resistance is a problem as seven per cent of cases show multidrug resistance. More than new patients, relapsed patients are more susceptible to this and there is 11 to 15 per cent of relapsed cases.
But, the problem first arises from irregular drug consumption. So, in the post-Covid scenario, we have planned more nutritional programmes. We are also giving Rs 5,000 extra allowance to those with the poorest of economic status and those affected by the pandemic, Meanwhile, we are also giving health workers additional allowance for their work in community health facilities so that they can oversee patients consuming drugs regularly.
What about the budget for R&D, human resources and programmes?
Regarding the five-year plan, the estimated budget is Rs four billion. But, through the plan, we are trying to set up a one-door policy to get financial help from all donors and supporters.
Regarding the research, funding is more on need-based things rather than proactive research. But, small-scale research is funded by the organisation itself. The NTCC is also holding more lab-based testing with culture and gene-based research. Other irregular research and in-depth study are held in collaboration with SAARC and other international organisations.
For the next fiscal year, the NTCC is starting a survey to further study and analyse the trends of tuberculosis in Nepal. Throughout the time, we will also be setting up biometric identification cards to get a real-time update and minimise the plurality in cases.
Overall, what can expedite Nepal’s progress to curb tuberculosis?
The NTCC is working towards ending tuberculosis in Nepal, but it is not a one-party effort. All tiers of the government, national and international health organisations, EDPs and people need to work together.
The federal system changed the much needed vertical chain of command. So, now, the local level has to be more active and take ownership, prioritise and commit to holding different programmes and allocating budget. After all, the local governments can facilitate first-hand diagnosis and treatment better. It has to initiate and ask for facilitation where needed rather than wait for external support or intervention.
Further, according to the five-year plan, we will first take DOTS centres to each municipality so that it can minimise and track family and community-based infection. Secondly, we will hold in-patient and other training and facilitate better treatment. And third, we will bring all the pending organisations into the network and facilitate them.