
Many people tell women in Nepali society that motherhood completes them. One of the first things a new mother does, after delivering the baby, is to breastfeed them. But, many children are not breastfed within the first hour of birth as recommended. Acknowledging the growing problem, Paropakar Maternity and Women’s Hospital has now started Nepal’s first human milk bank on its premises.
The milk bank hopes to increase the number of children breastfed in the first hour and consequently increase their immunity. The biggest maternity hospital in Nepal believes the new initiative can be a lifesaver for children and mothers who struggle to produce milk as needed.
Here, we will explain why the milk bank is needed and how the hospital plans to operate it in Nepal.
How did the milk bank idea come to Nepal?
Though needed, the milk bank concept entered Nepal late. The first milk bank started in Vienna (Austria) in 1909, then in Massachusetts (the USA) in 1919. Nepal’s immediate neighbour India began it in 1989 and now has more than 80 milk banks.
Amir Babu Shrestha, Director of the hospital, shares that the hospital felt the need for the milk bank given that there was a decrease in the breastfeeding culture among new mothers. “The talks started last year. We felt the need for the milk bank and we sent a team to Delhi, India, where they researched and did the feasibility study in Nepal’s context.”
Why is it needed in Nepal?
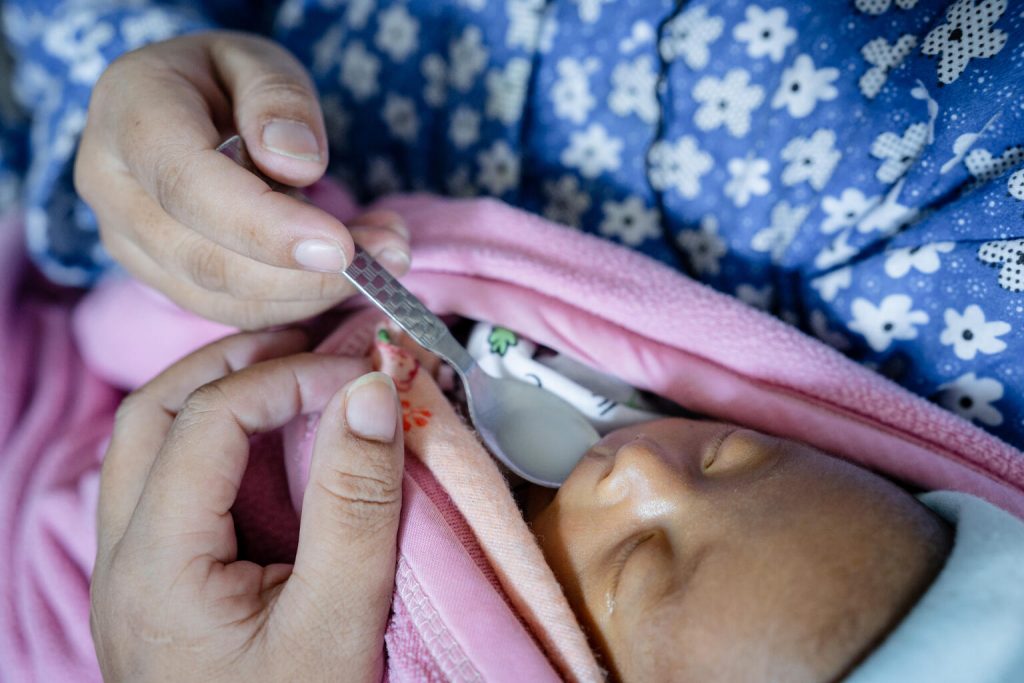
Shrestha shares, “If the children are breastfed as recommended, we can decrease the infant mortality rate by over 30 per cent and decrease the chances of diseases by over 20 per cent. So, we are trying to increase the access of all the newborns to breastmilk.”
“We saw women sharing that they cannot or did not want to breastfeed. Then, they either feed them powdered milk or bring them to the hospital seeking help. Some who chose not to breastfeed were concerned about their body and career. The working women also had to make the hard choice of not breastfeeding as they had to go back to their work. They choose to use breast pumps, which is also a good option.”
On the other hand, some women cannot produce milk. “Though we do not have data on Nepal, some 10 to 15 per cent of the mothers of the children kept in the neonatal intensive care unit (NICU) of the hospital could not produce milk.”
But, Shrestha says that is rare that women cannot produce milk because of some serious issues. “There is a condition called breast abscess, in which women see pus forming around the breast tissues halting the milk production. But, majorly when women cannot breastfeed, it is because the women do not know how to.”
“There are nurses in our hospital who counsel the new mothers and teach them how to massage their breasts so that they can produce the milk. And we will continue this in the milk bank too,” he adds.
To aid either of the mothers, the milk bank will increase the children’s access to breastmilk so that they grow healthy and disease-free.
“Just recently, we also celebrated the World Breastfeeding Week, from August 1 to 8, with the theme ‘Step Up for Breastfeeding: Educate and Support’. The milk bank also aligns with that.”
How will the milk bank function?

The hospital’s milk bank contains freezers and storage units to store the breastmilk for up to six months.
Shrestha, explaining the process, says, “The new mothers will be counselled by the nurses and with their consent, we will be extracting some 50 to 100 ml of breastmilk from them, at a time. The facility will have a separate safe space for women to breastfeed or pump the milk. We will collect the milk and test it for any kind of infection. If clear, we will collect it into one storage vault and mix it with other women’s breastmilk. The milk gets pasteurised, bottled and then stored in the refrigerator for up to six months.”
Is feeding other women’s milk beneficial too?
Mixed breastmilk does not have any negative impact on the children, he assures. “Though not in Nepal, research has shown that it will be completely safe for all children. It will have all the nutrients needed for the children. In fact, in Nepal, there has always been a trend where women share their breastmilk with children from another mother when they need it.”

According to Kalpana Upadhyaya Subedi, the chief consultant paediatrician at the hospital, “We mix the breastmilk of three to five mothers, as recommended. Mixing allows the breastmilk to have all the nutrients, collectively, that one mother might lack. So, it will be more nutritional for the babies.”
Can all moms benefit?
The milk bank, for now, is limited to the patients admitted to the hospital. Shrestha says the hospital, however, plans to expand the services to all with time. “It is a human product, so we plan to distribute the milk to the mothers, as needed, free of cost. It is a service so it will be and should be free all the time.”
The milk bank will be operated by a team of six people and is being operated under the government’s budget along with technical support from UNICEF.

























