
After giving birth to her first child 11 years ago, Srijana Budhathoki could not breastfeed her child for the recommended six-month period. There were two major reasons: first, her physical inability to produce sufficient milk, and next, her having to return to her work in less than two months of the parturition.
“As I could not produce milk for the baby while at the hospital, the nurses there recommended I feed the baby Lactogen (a whey-based milk powder). Then it became a norm, as the baby would not suckle on my breast and prefer Lactogen over whatever little breastmilk I could produce,” she adds.
With several women suffering problems like Budhathoki, breastfeeding in Nepal has been declining for decades now. In 1991, the Nepal Demographic Health Survey (NFHS) found that only 22 per cent of children were breastfed within one hour of birth. But, recent data show almost all babies are breastfed but only 18 per cent are breastfed within one hour of birth as recommended, and over 60 per cent are breastfed within the first 24 hours.
National data also reports that breastfeeding frequency and tradition are decreasing due to different reasons. In 2011, it was reported that 70 per cent of mothers breastfeed. In 2016, it decreased to 66 per cent and in 2019, it reached 62 per cent, causing alarms among public health workers and stakeholders.
Insufficient maternity leave
Budhathoki was working as a senior croupier at the Everest Casino during her first childbirth, and she was asked to return to work after 52 days of maternity leave. “I had to leave the baby with my mother and my sisters at my parents’ home. The baby was used to being with my mother and would not seek me while I was at work. The time to bond with my child was certainly less.”
It has been over a decade now, yet, why Budhathoki could not breastfeed her child is still a story of many working women today.

On paper, Nepal has definitely made some striding efforts. At the national level, the government has recognised the plight of working women and extended maternity leave to 14 weeks, as stated in the Labour Act, 2017 (section 45). The Right to Safe Motherhood and Reproductive Health Act, 2018 (section 13) also maintains that working women are subjected to an obstetric leave of up to 90 days. Women are entitled to two months of paid leave, one month of unpaid leave and an additional one month of unpaid leave in case there is a doctor’s recommendation.
Following that, some employers have started practising it. “I got two months of paid and one-month unpaid leave,” remembers community medicine expert Dr Mukta Singh Bhandari.
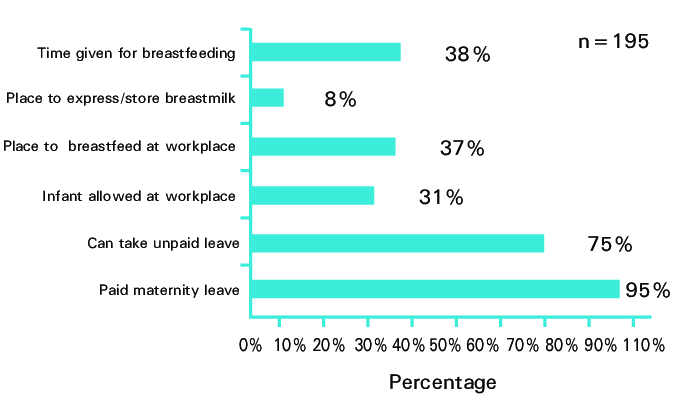
Meanwhile, after her experience, Bhandari conducted a study on this very subject in 2017. “Though almost all women got maternity leave, only 75 per cent got an additional one month of unpaid leave,” she remembers. But this means that women, who got maternity leave, can breastfeed only for three months and not six months.
Among many private institutions, the right is not secured on the grounds that not everything that the law mandates are possible to implement. The argument has led many to shrug off the provision and deprive women employees of the leave, according to Forum for Women, Law and Development, an organisation that works for women’s rights in Nepal. The reasons why institutions deny maternity leave are numerous.
And experts view a limited period of maternity leave will have a direct impact on breastfeeding.
“There are two types of breastfeeding that one can do: scheduled and on-demand. While scheduled breastfeeding has been proven to be better for the mother’s physical and psychological health, the child’s IQ development has been low in this case. On the other hand, the on-demand model is proven better for a child’s development but it is likely to increase depression and exhaustion among mothers,” explains Bhandari. But, sadly, either is not possible for working women after they resume work.
“About 31 per cent of women chose or were compelled to choose to go back to work rather than take time and continue exclusive breastfeeding at home. Those who continued breastfeeding after the resumption of work lacked the organisational structure where they could express breastmilk and store them properly,” Bhandari explains the results of her research.
Infrastructure crisis
When it is impossible for women to directly breastfeed the kids, expressing and storing breastmilk is a solution. But, there are some problems in terms of infrastructure to practise that in Nepal.
Expressed breastmilk needs to be stored in a refrigerator at a specific temperature of 40 °F (4 °C) for four days and in a freezer at 0 °F (-18 °C) or colder for up to six months. Before feeding, the milk needs to be heated in hot water, together with the bottle.
Hospitals or big-budget organisations have the resources to provide their female employees with space or resources for the purpose. However, not all offices have bothered or prioritised the need for space for women. “The office has not thought of the need for such because we have a younger female workforce who is unmarried and not expecting,” says a woman, seeking anonymity, based on her experience at a Kathmandu-based NGO.
Whereas expecting or new mothers are expected to maintain the decorum and timings of the office. This coupled with no space for breastfeeding or a lack of daycare is compelling women to leave their child(ren) at home and discontinue exclusive breastfeeding, though recommended.
Radha Paudel, the founder of the Global South Coalition for Dignified Menstruation (GSCDM), says it is Nepali employers that are unwilling to make such changes and denies it is a budget problem. “It all depends on the employer or the office and their commitment and understanding to make their employees comfortable. First of all, the employers need to get a clear understanding of gender equality.”
“When I conducted training for women in Hetaunda some 11 years ago, the group had new mothers too and we made sure that the women were comfortable. We hired locals to babysit for them while the training was ongoing. So, when the babies needed to be breastfed, the mothers would go and do that easily. Other older children were kept busy with toys,” she says, adding it is an international practice already and should be adopted here widely too.
“Working women prefer not taking their children to the office as their work can get hampered. Offices should exclusively mention on their application forms and policies that new mothers will be taken care of so that they can have the confidence to join or resume working. Otherwise, women will continue to lose opportunities and lag behind, “punished” for choosing their babies over their work,” she adds.
Although Paudel agrees not all offices might be equipped enough to give all the services, she stresses the least the offices can do is give new mothers the flexibility to feed their babies in the morning and not rush to report on the dot. “The Covid-19 pandemic has taught us that physical presence is not as necessary as before. So new mothers definitely should get to enjoy and be privileged to work from home so that the newborns and the new mothers do not have to compromise on breastfeeding or the work.”
“Women in western countries are boldly and naturally breastfeeding their children even in public spaces. It is only here that we are hesitant and women feel embarrassed to be witnessed during this natural process,” Paudel says.

No alternatives
Experts say breastfeeding does not have any perfect alternative. Even traditional baby food of Nepal such as lito cannot work, says Dr Mukta Singh Bhandari, who claims her study showed working women in the past were feeding lito or solid food more than what was recommended.
Mother’s milk consists of immunoglobulin; it has been called the first vaccine for the child. Those who are breastfed for at least six or up to two years are reportedly more physically and mentally developed, their IQ is better and their jaw development.
Breastfeeding is not only good for babies but also for new mothers. “Regular breastfeeding significantly decreases ovarian and breast cancer risks in women. Their uterus can get back to shape quickly, maternal mortality decreases, and postpartum depression also decreases,” says public health expert Dr Aruna Uprety.
Exclusive breastfeeding is recommended for the first four to six months of a child’s life because breastmilk is uncontaminated and contains all the nutrients needed by the children. In addition, it provides some immunity to diseases through the mother’s antibodies. Early supplementation, especially under unhygienic conditions, can result in infection and lower immunity to disease.
In children who have not been breastfed as recommended or at all, there are higher chances of developing lower bodily growth and compromised mental capabilities. “Other common problems are bronchitis and getting regular colds, fever and diarrhoea or other digestive problems. Whereas those who were breastfed well show early signs of brain development; they start to sit, walk and talk earlier than others,” explains Poudyal.
To continue feeding breastmilk, one option for working mothers is expressed milk in bottles. But, Dr Uprety observes working women from the informal sectors are still way behind in enjoying this privilege. Those working also do not have access to breast pumps to fasten the process.
Meanwhile, the experts also warn women against using formula feed for their babies. “The use of the formula is risky as it has a health impact on the infants, especially premature babies. So, nothing can replace breastmilk for babies,” says Bhandari.

Uprety also seconds that the aggressive marketing of Lactogen is unethical and causes harm to both mothers and babies. “Nurses at the Prasuti Griha (Paropakar Maternity and Women’s Hospital), where I worked in the 1980s, were recommending Lactogen. But, the bottle nipple is more addictive for babies and it discourages babies from suckling on their mother’s breasts. So, the hospital and many others have banned recommending it. However, it is not true everywhere.”
In cases like that of Budhathoki, where mothers cannot produce breastmilk, this can be seen very often.
Dr Prithuja Poudyal, a paediatrician at the Dhulikhel Hospital says, “In such cases, mothers are taught how to massage and how to angle the breast and how much of the breast area the baby should suck. Lactogen and bottle feeding should be discouraged, but those who choose childbirth at home and community healthcare centres do not get that recommendation.”
“In some cases, new mothers are in ICUs or babies in NICUs and mothers are not able to produce milk, the hospitals also recommend they feed the babies breastmilk of other new mothers and not Lactogen. There might be a risk of HIV and hepatitis, but hospitals are equipped to check this so the process is safer.”
While expressing and storing breastmilk is recommended, Poudyal does not recommend the use of breast pumps. “Breasts produce milk because of an oxytocin reflex that is stimulated. So, the use of breastmilk does not increase milk production. In fact, breast pumps can be harmful as they can hurt the breasts, increasing stress.”
Meanwhile, bottle-feeding can shorten the period of postpartum amenorrhoea but increase the risk of illness, diarrhoeal disease, and infection if one fails to sterilise them properly.
Originally published on August 1, 2021
























