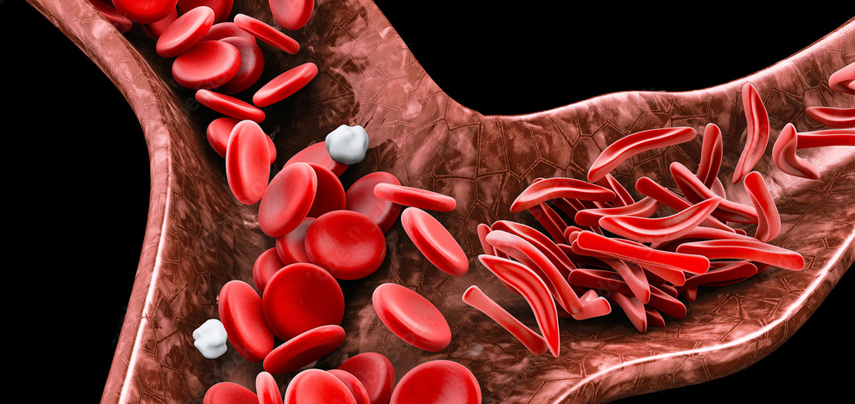
Sickle cell disease is an inherited blood disease, which causes an abnormality in the oxygen-carrying protein haemoglobin found in red blood cells, leading it to a rigid, sickle-like shape. Under certain circumstances, it can result in multi-organ damage, severe pain, increased risk of infection, and even death if not managed appropriately.
Sickle cell disease is seen when a person inherits two abnormal copies of the β-globin gene (HBB) that makes haemoglobin, one from each parent. The person is termed as a “carrier” if he has a single abnormal copy of HBB and is said to have sickle cell trait but usually no symptoms. The problems in sickle cell disease typically begin around five months of age and an average life expectancy for them in the developed world is 40 to 60 years.
In the past, the disease troubled Nepal, in particular, the Tharus living in the southern belt of Nepal, so much so that it was called a nightmare for them. So, what is the situation today?
Prevalence around the world
As of 2015, there were about 4.4 million patients with sickle cell disease, while an additional 43 million were seen to have sickle cell traits. Likewise, 114,800 deaths of patients were observed in 2015.
About 80 per cent of sickle cell cases are believed to occur in sub-Saharan Africa.
It also occurs relatively frequently in parts of India, the Arabian Peninsula and North Africa, then to a lesser degree in Southern Europe and Asia Minor and among people of African (sub-Saharan) origin living in other parts of the world.
Sickle cell disease in Nepal’s context
While talking about Nepal, the Tharu people are predicted to have a higher prevalence of sickle cell disease than the rest of the Nepali population. The prevalence of the disease has grown among the Tharu people because of the tradition to marry within their own tribe as sickle cell disease is a recessive trait and requires both parents to carry the gene.

According to a 2017 study, to estimate the prevalence of Hb S (HBB: c.20A>T) among the Tharu population in the rural district of Dang in Western Nepal, 9.3 per cent screened positive. After the diagnostic gel electrophoresis testing of 133 positive patients, 75.9 per cent were confirmed to be Hb AS heterozygotes, 4.5 per cent were confirmed to be Hb SS homozygotes and 19.5 per cent were false positives. This shows a large burden of sickle cell disease in the Tharu community, for which allocation of appropriate resources and proper management should be done.
According to Dr Shraddha Lamsal, there is a 75 per cent chance for children to suffer from this disease if both of their parents are suffering from it whereas the chance of infection is about 25 per cent among them if only one of their parents has the disease.
Symptoms
The attack of sickle cell disease is triggered by temperature changes, stress, dehydration, and high altitude. The symptoms of the disease vary from person to person and can change over time.
Some of the common early symptoms of this disease are yellowish discolouration of the skin (jaundice) or whites of the eyes (icterus), fever, shortness of breath, extreme tiredness or fussiness from anaemia and painful swelling of the limbs.
Its complications can be severe such as delayed growth and puberty, infections, joint problems, acute and chronic pain, pregnancy problems, acute chest syndrome, enlarged spleen, eye problems, gallstones, heart, liver and kidney problems, leg ulcers, priapism, stroke or silent brain injury including aplastic and splenic sequestration crisis.
Diagnosis and treatment
The diagnosis of sickle cell disease can be done with the help of blood tests and genetic screening. We can also do prenatal screening of amniotic fluid or a sample of tissue taken from the placenta before the child is born.
In newborn babies, screening of the blood from a heel prick is done to identify whether the baby has sickle cell disease or its trait.
The treatment of the disease is symptomatic as well as specific.
Several medications should be taken for the prevention of the sickling of the red blood cells, vaso-occlusion, infection in the bloodstream and pain management. In some conditions, even transfusion, blood and bone marrow transplantation, as well as potential gene therapy treatments might also be required. The cost of such treatments is not a cup of tea for most of the citizens of developing countries like Nepal.
In 2014, the parliament of Nepal took up the issue of sickle cell disease and recognised it as a major health crisis in the nation by declaring it as a public health problem. As a result of that, patients with sickle cell disease can now receive government-sponsored treatment for up to Rs 100,000.
Awareness should be raised about the appropriate tests to timely identify the sickle cell disease in prenatal and postnatal stages, disadvantages of marriage within the same community and compulsory blood tests before getting married in the communities prone to the sickle cell disease.


























