
It has been two years since a five-bed intensive care unit (ICU) with a ventilator was set up at Jaleshwor Hospital in Mahottari. But, due to a lack of skilled medical personnel, the hospital has not been able to operate its ICU and it normally recommends its patients elsewhere.
To operate an ICU and the medical equipment there, the hospital needs at least one internal medicine expert, one anesthesiologist, four medical officers and 10 staff nurses. But, according to the hospital’s medical superintendent, Dr Satish Kumar Sah, it only has one permanent doctor, four staff nurses and six helpers.
“The provincial government helped up set up the ICU, but we’ve not been able to fill the vacancies needed to run it,” says Sah, adding the hospital cannot operate the ICU with the people it currently has.
Myagdi’s Beni Hospital is in a similar state. The hospital has five ICU beds two with ventilators for adults and four ICU beds with two ventilators for children.
The hospital’s medical superintendent Dr Jitendra Kandel says out of 65 positions in the hospital, only 13 have been filled so far. During the Covid pandemic, the provincial and central governments helped the 50-bed hospital with medical equipment to set up an ICU. But, due to a lack of staff, the hospital has not been able to operate it.
“We work with so few staff members that it is hard for us to provide good service as more and more people come seeking help. It’s hard,” says Kandel.
The local government had employed 30 temporary medical professionals at the hospital. These people have been removed since June and this is causing major issues at the hospital as it can not provide ICU and ventilator services to those in need.
This is a story in most hospitals in the country except those located in key cities. This is why Nepal’s health sector was proven to be weak during the Covid pandemic. The hospitals lack a proper system, do not have the infrastructure and most do not even have the human resource to operate the available medical equipment to provide services to people.
Availability of medical equipment
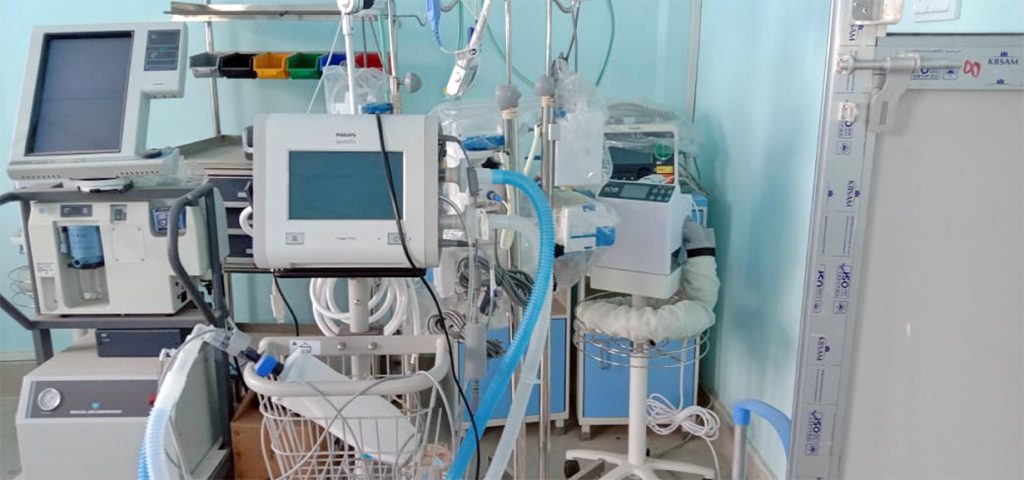
In a bid to save the lives of people, the government sends medical equipment to most hospitals, but due to a lack of staff, they lie idle, gathering dust.
According to the Department of Health Services, the country received a lot of medical equipment from donors during the Covid pandemic. It received 9,196 oxygen cylinders, 440 ICU beds, 711 ventilators, 305 CPAP machines, 788 BiPap machines, 66 electronic beds and 2,570 infrared thermometers from donors.
The government distributed most of the equipment across the country on a needs basis, says Rudra Prasad Marasini, the chief of the Management Division there. But, he says despite sending it, the government has not monitored its state.
“The central government cannot monitor if it’s being used. We are responsible for sending people, but we have no idea if the equipment is being used or not,” says Marasini.
According to the Ministry of Health and Population, in June 2020, the country had 528 ICU beds and 222 ventilators. As of June 2022, that has increased substantially as hospitals across the country have 2,797 ICU beds and 1,008 ventilators.
This shows the government took efforts to improve health facilities in the country but it did not focus on increasing the number of human resources to operate the available medical equipment.
Lack of monitoring
During the Covid pandemic, the government recruited additional health officials on a contract basis across the country. But, as the pandemic has subsided, the government has decided not to renew their contract leaving hospitals understaffed.
Take Sukraraj Tropical and Infectious Disease Hospital as an example. This hospital has not been able to use its ICU fully and is referring people to Bir Hosptial.
During fiscal years 2020 and 2021, the Infrastructure Division of the Department of Health Services monitored around 50 hospitals in the country. In the monitoring, it came to the conclusion that most hospitals have more medical equipment than necessary.
“Hospitals don’t have a place to keep some medical equipment. Then, they have to store some of the equipment as that cannot be used because of lack of skilled staff,” says bioengineer Sajita Sharma.
The country is currently going through the fourth wave of Covid. In total, nearly 12,000 people have lost their lives to the virus. There is enough proof to say a lot of people died because they could not get an ICU bed or a ventilator or other medical equipment.
The government in the fiscal year 2020/21 set aside a budget of Rs 6.99 billion to buy medical equipment. But, the report prepared by the Office of the Auditor General states that the government has not prepared a list nor has it monitored the equipment that was purchased and sent out to various hospitals.
The report also states that organisations like National Ayurved Centre, Prasuti Griha, Civil Service Hosptial, Patal Hospital, Gajendra Narayan Singh Hospital and Bheri Hospital did not buy HDU medical equipment fairly.
Short-sightedness in sight
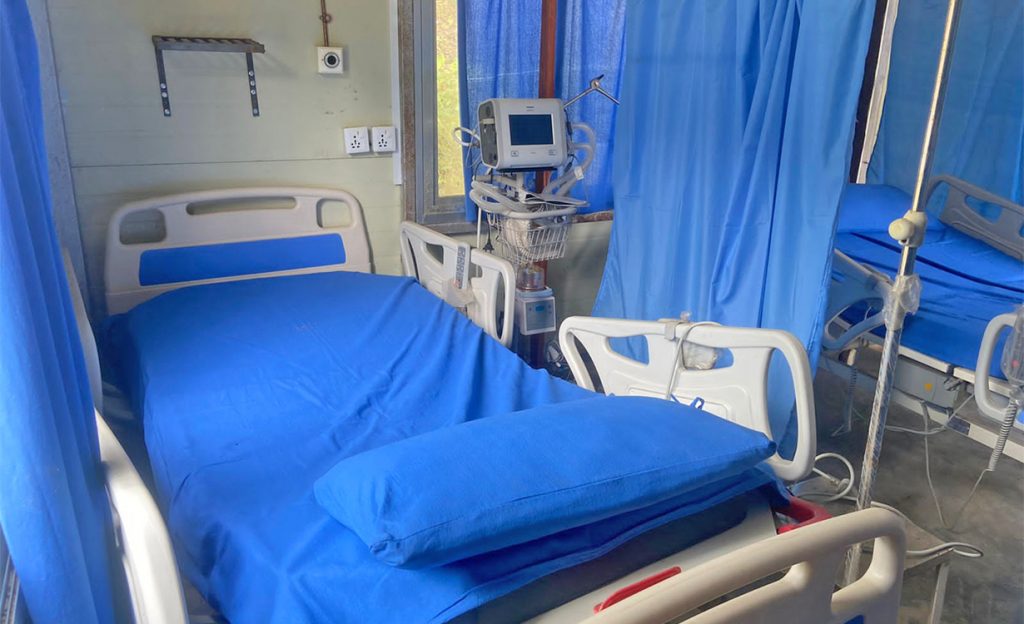
Using the condition of the Covid pandemic, various government departments and hospitals at different levels bought a lot of medical equipment. But, most of the equipment is in a useless state.
This, experts say, is due to the short-sightedness of everyone involved as they did not think about needed skilled human resources before buying the equipment.
There are so many examples of this in the auditor general’s report. Take BP Koirala Institute of Health Sciences, where an MRI machine is in a dormant state for months. The institute also has 15 dialysis machines not used due to a lack of people who know how to operate them.
At Patan Hospital, medical equipment like portable ultrasound, anaesthesia, ECG and oximeter are not being used as they need repair. At Bir Hospital, a tomotherapy machine bought for Rs 470 million broke down without it being used even once. The hospital without making a mechanism and not having the human resource bought the machine in 2017. In the five years since its purchase, the hospital has yet to install it.
The ministry’s former expert Dr Sushil Nath Pyakurel says the country should buy equipment based on human resource, infrastructure and need.
Other reasons
“The government has to first make a plan before buying any expensive medical equipment. But, having not done that, we now have a lot of expensive equipment gathering dust at hospitals,” says Pyakurel.
He says the reason homework is not done during the purchase of this equipment is the greed for commission and political selfishness.
“Everyone wants their cut, but they don’t even see if there is a need,” says Pyakurel, adding he saw medical equipment worth Rs 2 billion go to waste during his time as the director general of the Department of Health Services.
Health ministry officials themselves agree that the equipment they send to rural areas of the country has not been used. For that, they blame the lack of skilled human resources.
“We should have accepted the medical equipment donated by foreign agencies by first thinking if we need it or not. But, we never did that and accepted everything and that resulted in us taking some equipment that we didn’t even need,” says Dr Kiran Regmi, a former secretary of the Health Ministry. “Now, a lot of medical equipment in the country is lying idle.”
The biggest problem

The pandemic has taught Nepal a valuable lesson. When there was a need, the country did get all the medical equipment it needed. But, the country could not manage human resources.
The government has permanent positions for 1,650 doctors, but there are currently only 1,400 doctors working for the government. Of them, 500 are specialists and 900 are medical officers. The total number of government anesthesiologists is only 80.
The pandemic gave the country a chance to change this and improve the health sector. But, nothing was done to improve it, says Nepal Medical Association President Dr Lochan Karki.
“We’ve been requesting the Health Ministry and the prime minister to help develop skilled human resources. But, they just don’t seem to care. This is such a pity,” says Karki.
The number of government doctors the country needs today has not changed since 1992 when the population was 20 million.
“Nepal has 30,000 registered doctors, but still, the total positions the government has is 1,400. I feel this is embarrassing. How long will 1,400 doctors sustain a growling population like Nepal,” questions Karki.
The government is planning to set up basic hospitals in 659 local governments and provide services, but despite that, it has not talked anything about increasing the number of positions for doctors.
“Unless the government increases the number of health professionals, nothing will change despite having a lot of medical equipment,” says Karki.
TU Teaching Hospital’s ICU chief Dr Subas Acharya says it is time that hospitals in the districts worked on a referral basis as he says it will take almost a decade to send skilled medical professionals to all hospitals in the country.
“We have to work with what we have because it takes a lot of work to produce people who know when a patient needs ventilators,” he says.
These decisions can only be made by a medical consultant who has a master’s degree in internal medicine or anaesthesia. The doctor also needs training in critical care, which takes up to three to four years to be called an expert. “These can’t be created in a day.”
This is because Nepal has only 35 doctors who are experts in critical care.
“We should stop saying we have built a 20-bed ICU at district hospitals. We don’t have enough people to operate medical equipment there,” says Acharya.
Dr Hemraj Paneru from the Nepalese Society of Critical Care Medicine (NSCM) says the government not thinking about how the ICU works is wrong.
“It’s easy to buy equipment. But, we need to understand people who can use them aren’t born overnight. The government’s focus should change,” he says.
The ministry knows this and says it will train the medical professionals at district hospitals on how to use the equipment there.
“We don’t think we need a person who’s done masters at all hospitals. That’s not financially practical too but we can train those who are there on how to use it,” says Dr Sameer Kumar Adhikari, assistant spokesperson at the ministry.
“We understand how overworked health professionals are in the country. We are looking at increasing the number of doctors at the government level, but until then, we will hire them on a contract basis,” says Acharya.
—
This story was translated from the original Nepali version and edited for clarity and length.

























