As a student of ophthalmology and later as a glaucoma expert, something always bugged Suman Thapa. A general consensus among ophthalmologists was that they should not test for ailments, with a low prevalence rate, that they couldn’t treat affordably; and glaucoma, the second biggest cause of blindness after cataract, was one of them.
One and half decades later, he is doing what he was told not to. “They used to say that we should not screen people for glaucoma because the chance of it getting treated is very low. Also, its prevalence was low, but the costs involved in the diagnosis were high. They thought diagnosing disease and failing to provide a cure for it is unethical for a doctor,” Thapa recalls his student life in the mid-2000s.
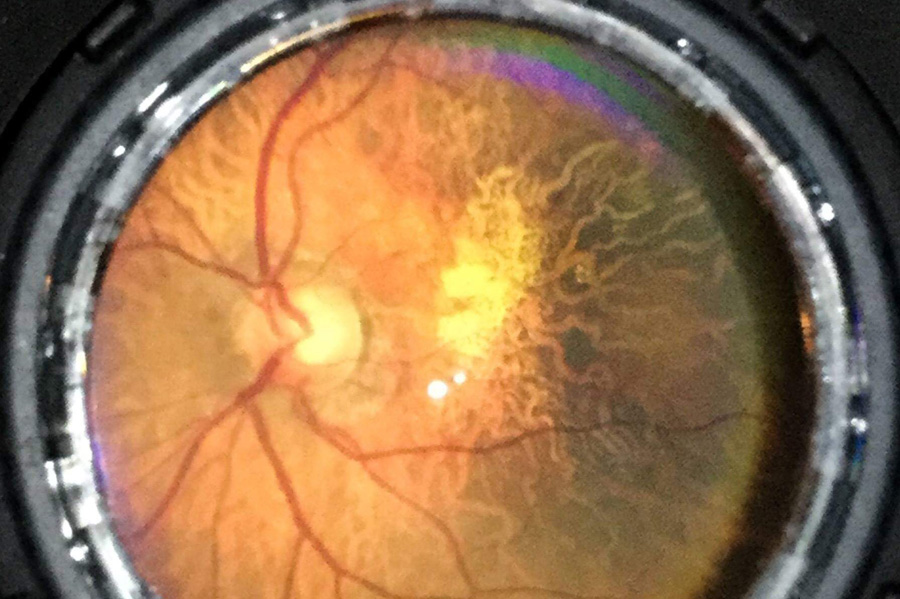
“But, I used to argue that it was wrong because glaucoma blindness is preventable if we diagnose it during its early stage. I believed that if we could capture images of optic nerve inside people’s eyes in a cost-effective way, we could catch glaucoma early and this could be a great start towards preventing blindness caused by the ailment.”
With this belief, Thapa began exploring ways to find easy and affordable tools to photograph the optic nerve. Today, he has reached halfway.
A team at Tilganga Institute of Ophthalmology under Thapa’s leadership has proved that a pocket-sized tool can be used with mobile phones to catch the ailment which gradually makes a person blind.
“What we have developed is one of the easiest and most affordable tools in the field of teleophthalmology (the use of telecommunications in treatment of eye diseases) in the world,” says Thapa whose team is working further to make the tool more user-friendly. He hopes that such tools can be instrumental in providing healthcare to the rural population in countries such as Nepal where trained ophthalmologists are not available in rural areas.
The tool and its adaptation in Nepal
Thapa, the current head of the Research Department at Tilganga, one of the biggest eye hospitals of the country, was in Vancouver for an academic event in 2012. During a casual conversation with John Hopkins University professor Alan Robin, he said that eye screening tools should be portable, cheap and easy to use for non-doctor technicians so as to serve the rural population.
“Then, Professor Robin introduced me to Chris Johnson, an ophthalmic tool designer. Fortunately, Robin also knew that some people had been using a 5,000 dollar camera with an iPhone,” the smiling doctor shares, “Then, I proposed testing its validity by comparing its performance with optic cameras that cost as much as $40,000 .”
The test was successful. Thapa shares, “We published success stories in many international medical journals and received appreciation from the international ophthalmologic community.” After that, Thapa proposed that the tool be used in a real setting. He shared with his international colleagues that Nepali villages did not have ophthalmologists, but there were trained technicians working with the rural population; and he wanted those technicians to test the efficiency of such tools to make decisions about referring cases to doctors for further diagnosis.
“Let’s give this camera to the technicians and send them to a village, say in Manang. The technician has to see people’s eyes through this camera and send the report to the ophthalmologists at Tilganga,” he recalls his proposal. The team members agreed. But, before they implemented their plan, the mega earthquake rattled the country in April 2015, forcing the team to defer the plan. The country took nearly a year to get back to normalcy.
While Thapa was thinking of beginning fresh efforts to use the 5,000 dollar camera in eye screening in rural Nepal, he was invited by Stanford University to give a talk on teleophthalmology in Nepal. During his sojourn in the US, some researchers at Stanford told him that they had a tool named ‘Paxos Scope’ that can be connected to any Apple device to screen eyes.
“They showed the tool to me,” he says, “It was a small tube; you could keep it in your pocket.”
Another plus point was that the tool was already validated and the quality of photographs captured with the device met the clinical standards. “If you talk about the price, all the components of this device cost less than 500 dollars altogether,” he says, “This is way cheaper than you had imagined.”
Then, Thapa decided to take the tool to Nepal and test its effectiveness.
The pilot study

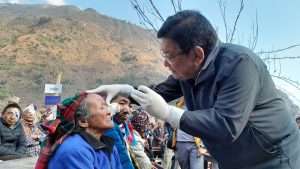
Back from Stanford, Thapa organised a training programme for rural technicians of community eye centres, operated by Tilganga hospital, across the country. The group primarily consisted of young people who had received a three-year diploma course from the Council of Technical Education and Vocation Teaching after completing of their high school.
Their job was simple: check people who visit their centre, treat minor cases with general medicines and refer serious cases to the hospital.
After training the technicians, the hospital selected four sites for the pilot study: community eye centres in Jiri, Charikot, Dolakha and Ramechhap of central Nepal. The staffers at these four stations were given an additional responsibility: besides deciding preliminary treatment and referrals, they now had to take pictures of optic nerve of the patients and send the images to the hospital. Then, the ophthalmologists of the hospital had to decide if the patients needed any referral based on those high-quality images.
Comparing the referral decisions made by the two groups, it was found that the number of cases referred by the doctors was 20 per cent higher than the number of patients referred by the technicians. “It means the 20 per cent people would have missed the required treatment if this camera was not available there,” he says, “It proves that the need for this device is real in rural Nepal.”
Over a period of ten months, the technicians had screened eyes of 346 patients with the Paxos Scope and recorded the images.
Expansion

Currently, the Paxos Scope works with Apple devices only. The technical team of Tilganga Institute is currently working to make an Android-friendly version and develop its own app so that it can be more accessible.
In the meantime, the hospital has distributed the device to additional 11 community eye centres for their daily use so that they can make better decisions regarding diagnosis and referral. It has been used in some community outreach programmes of the institute also.
As the research is still underway, he hopes that further developments will benefit the larger public. Though it was intended to help people suffering from glaucoma, the tool has been useful for other patients also.
Meanwhile, Thapa is happy that his efforts, though they contradicted established norms of the discipline, are likely to prevent blindness in thousands of people in the country.
Photos: Courtesy Pradeep Banjara/TIO