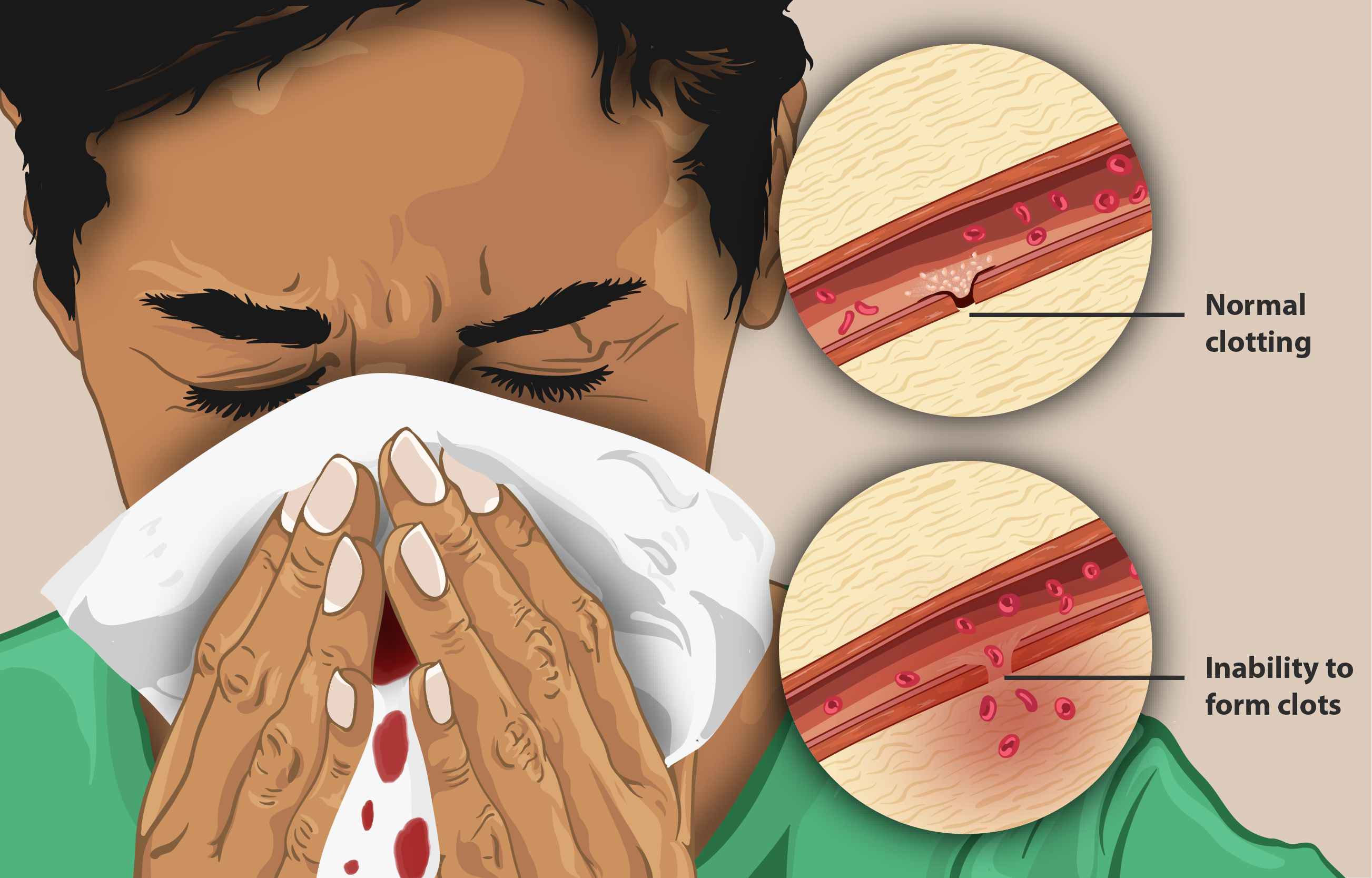
Haemophilia is a rare but mostly X-linked recessive hereditary disorder in which bleeding does not clot or stop due to the lack of clotting factors VIII and IX. As a result of this, people bruise easily, experience prolonged bleeding after injuries, and are more likely to experience internal bleeding into joints or the brain causing permanent damage to the joints, long-term headaches, seizures, or a decreased level of consciousness.
According to the annual survey done by The World Hemophilia Federation in 2021, there are more than 234 thousand people suffering from haemophilia in the world. Among them 186 thousand people were found to be suffering from Haemophilia A alone, about 90 thousand people were living with Von Willebrand disease and around 18 thousand people with other platelet disorders. These numbers were published two years ago and might have significantly increased in 2023.
According to the Hemophilia Federation of India, haemophilia is usually inherited genetically but sometimes rarely due to a mutation in the gene and about one in every 5,000 males is born with the disorder in India. But, according to the Nepal Hemophilia Society, haemophilia occurs predominantly in males with an occurrence rate of one in 10,000.
In Nepal, there are around 850 people diagnosed with haemophilia. According to the National Population and Housing Census 2021, there are about 5,000 haemophilic patients in Nepal. This fact suggests that more than 4,000 haemophilic patients are out there in the community without the knowledge of the Nepal Haemophilia Society and living without the proper management and treatment of their condition.
Symptoms and transmission of haemophilia
The symptoms of haemophilia can range in severity from minor to major bleeding episodes. Common symptoms include severe bleeding after dental operations or surgeries, prolonged bleeding after injuries, spontaneous bleeding into joints and muscles, and easy bruising.
Haemophilia is predominantly a hereditary disorder brought on by mutation in the clotting factor-producing genes. Haemophilia A is caused due to the clotting factor VIII deficiency, whereas Haemophilia B results from a factor IX deficiency.
The prevalence of haemophilia A is about 1: 5,000 newborn males whereas, haemophilia B is about 1: 20,000 newborn males.
While talking about the mode of transmission of haemophilia, it is crucial to comprehend the occurrence of haemophilia. Haemophilia has an X-linked recessive inheritance pattern. Males have one X and one Y chromosome, while females have two X chromosomes.
A female who has a defective gene on one of her X chromosomes is considered a carrier but typically shows no symptoms. However, because men only have one X chromosome, they will develop haemophilia if they receive the defective gene from their carrier mothers.
Besides that, haemophilia might still be seen in people without any family history. About 30 per cent, or one-third, of haemophiliacs, do not inherit the condition from their parents. Rather, they suffer from haemophilia due to a mutation in their gene. This indicates the seriousness of haemophilia and needs to draw the attention of the concerned authorities to prevent, treat and manage it properly.
Based on the symptoms, risk factors, medical and family history (urine or stool colour, family history of bleeding disorders, bleeding events, or blood clots, frequency and duration of bruise or petechiae or bleed etc.), physical examination, and diagnostic tests (CBC, aPTT, PT, BT, CT, PT, INR, Clotting factors test, Bethesda test, etc.), a physician may diagnose the bleeding problem and determine whether it is hereditary or acquired.
Several strategies are used to control haemophilia, each one very specific to the patient’s requirements. Some of them are:
- Replacement Therapy: The primary objective of replacement therapy is to substitute the insufficient or missing factor by injecting the clotting factor concentrates, fresh frozen plasma and bypassing agents as a prophylaxis or on-demand treatment.
- Prophylactic Treatment: The incidence of bleeding episodes can be considerably decreased with regular factor infusions for prophylaxis irrespective of the on-demand treatment protocol, minimising joint injury, avoiding unnecessary surgical procedures and enhancing overall quality of life.
- On-Demand Treatment: Acute bleeding episodes can be managed by administering clotting factor concentrates as per the on-demand treatment protocol of haemophilic patients.
- Modern Novel Therapies: Birth control pills, vitamin K supplements, antifibrinolytic agents (such as tranexamic acid), and Desmopressin (DDAVP) were commonly found to be used for the treatment of haemophilia. However, along with the advancement of medical science and technology, different innovative treatments that target different aspects of the coagulation cascade are widely used in hemophilic patients to promote haemostasis. Medicines such as Fitusiran (by silencing RNA for Effective Coagulation Control), Emicizumab (a Monoclonal antibody that works by targeting Tissue Factor Pathway Inhibitor), and Concizumab (by targeting Tissue Factor Pathway Inhibitor) have transferred landscape of haemophilia management.
- Gene Therapy: By injecting functional genes into the body of a haemophilic patient to produce the lacking clotting factor, developments in gene therapy promise to deliver a long-lasting solution. Many South Asian countries such as Nepal and India are actively participating in different clinical trials on gene therapy for the solution of haemophilia.
Prevention and Education

Prevention of different complications of haemophilia is a vital goal. Key prevention strategies include:
- Regular Checkups: Visiting specialised haemophilia treatment centres regularly for monitoring and adjusting factor replacement therapy can prevent further damage and reduce bleeding.
- Joint Care: Providing proper education about the best joint care techniques can prevent haemophilic patients from severe joint bleeding, which can lead to long-term damage to the joints.
- Injury Prevention: The haemophilic patients should be educated about minimising the risk of injuries and managing bleeding in case of accidents.
- Psycho-social Support: Different programmes should be offered related to psychological support to the haemophilic patients and their families by the government and haemophilia societies in order to support them in coping with the challenges of living with haemophilia and its complications.
Complications of haemophilia
One who is suffering from haemophilia is prone to complications, which are listed below:
- Joint damage and haemophilic arthropathy
- Inhibitors and treatment challenges: Inhibitors are some specific antibodies that neutralise the effects of clotting factor infusions and pose a significant challenge for haemophilic patients by complicating treatment, making it less effective and increasing the risk of severe bleeding. About 30 per cent of individuals with Severe Haemophilia A and 1-6 per cent of individuals with Haemophilia B develop inhibitors.
- Chronic pain and it’s psychosocial impact
- Central nervous system bleeds
- Gastrointestinal and muscular bleeds
- Gastrointestinal and muscular bleeds




















