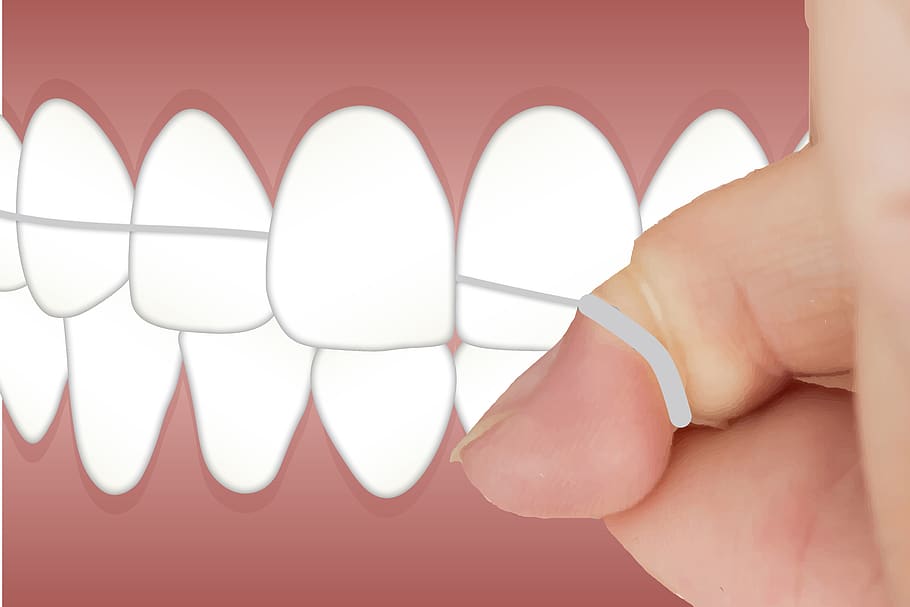
In December 2019, a pneumonia outbreak started in Wuhan, China. Later, it was concluded that the virus is a member of the coronavirus family and can cause infectious respiratory disease. This led to the Covid-19 pandemic.
The pandemic has become a challenge for health workers. Although it is not directly related to dentistry, dentists are also affected by the pandemic. Experts have said dentists are also among the front-liners who are at risk because they deal directly with the patients. Most of the equipment used in dentistry appears to have a higher survival rate making it risker to the patient as well as for the dentists. A noble coronavirus can survive for three hours in aerosol, four hours in copper, and 48 hours in stainless steel; it increases the risk of the infection among dentists.
Today when the outbreak of the coronavirus is at the peak, people should be aware of all the possible risk factors and preventive measures of the novel coronavirus and be safe. The safety of the patients and the doctors should be a primary concern and one must perform accordingly. Due to the characteristic of the dental setting, the risk of the spread of coronavirus among patients and dentists is highest. So, an effective infection control protocol is a must.
Clinics should avoid the crowd and clean the rooms frequently. Also, freshly sterilised instruments should be used. The doctor must check the temperature [must be >37.50] and the patient’s health status within the past seven days. The dentist should always wear a facial mask, wash hands frequently, and maintain a distance of a minimum of one metre from the patient. The patients also should only visit a dentist only if necessary and children needing an escort should maintain their distance.
Routine dental checkups have been reduced knowing the highest chance of transmission. In the case of elective care, treatment can be postponed for two weeks. For urgent care, pharmacological management (analgesics and antibiotics) must be the primary choice. In both cases, follow-up should be avoided in person. Instead, telephone calls and video conferencing can be done. But if it is an emergency condition, pharmacological management is a must. Dental treatment can be performed by using FFP2 and FFP3 (filtering face-piece particles) masks.
The dental process can cause the release of a large number of droplets and aerosols containing the coronavirus, especially when a person is in their incubation period or is unaware of the infection. So, the use of 0.2% povidone-iodine mouthwash prior to treatment can reduce a load of coronavirus in saliva. The use of a high-speed hand-piece and three-way syringe should be minimised as water coolants. When combined with bodily fluid, it can produce bio-aerosol. It can float in the air for a significant amount of time. On the other hand, the use of rubber dam scan reduces the splatting effect. Since small droplets can be a cause of transmission, airborne infection isolation rooms [AIIRs] can be used if the patient is suspected or confirmed with Covid-19.

Single-use disposals are the safest way for treating the oral area and should be encouraged. The possibility of the dentist being positive for Covid-19 and likely infecting the patient receiving treatment should also not be underestimated. Moreover, dental care should only be provided at a very crucial stage only, at least unless a vaccine is made available.