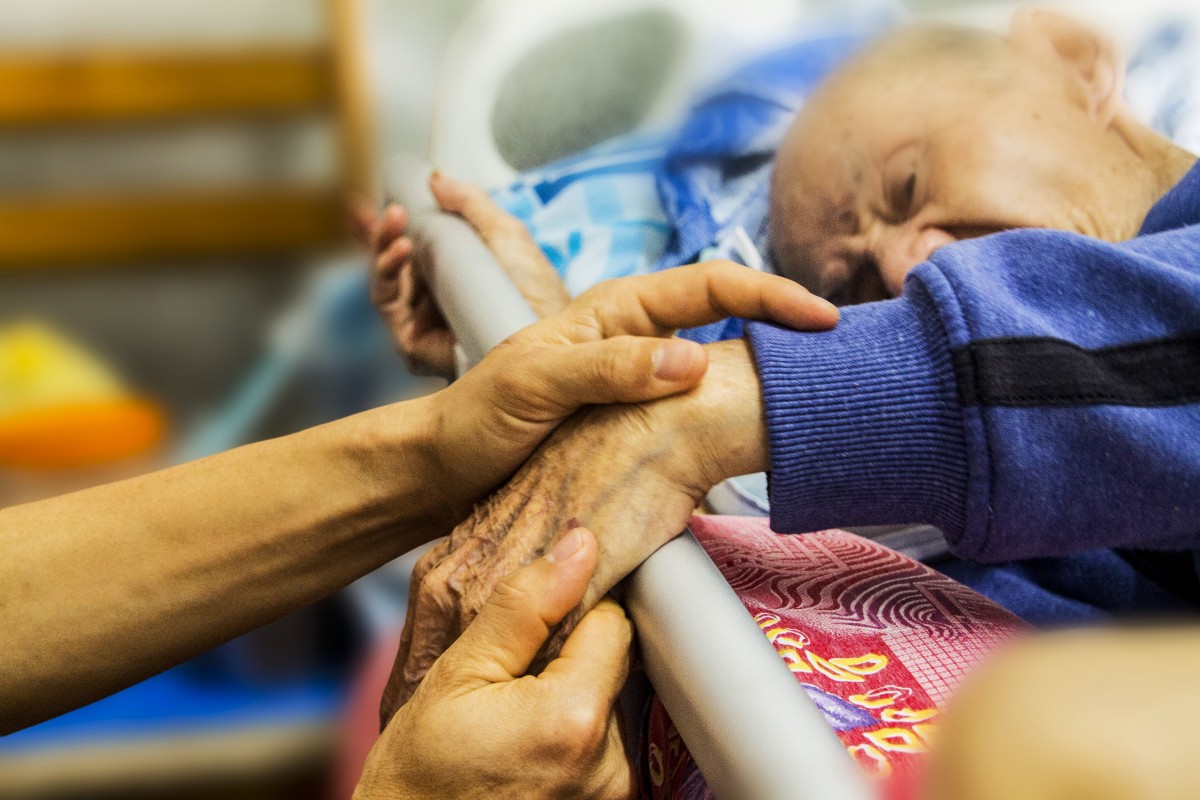
Abuse is the greatest concern in aged care facilities across Australia these days. People at these facilities are haunted with the question, “Who will keep me safe?”
The World Health Organisation (WHO) defines abuse as “a single, or repeated act, or lack of appropriate action, occurring within any relationship where there is an expectation of trust, which causes harm or distress to a person.” Generally, abuse occurs where there is a power imbalance between the perpetrator and the victim. However, surveys have found that most people who suffer abuse in aged care facilities are staff and residents. These cases are caused by acts perpetrated not by people who yield power over them, but those who lack power and are most at risk of abuse themselves.
Abuse of staff
Unfortunately, it has been accepted that caregivers experience a high level of aggression from other people in aged care facilities despite research highlights awareness of this problem spanning more than a decade. Sadly, some staff have accepted it as a part of the job. Staff who are constantly at risk of abuse from residents can become emotionally distressed and more detached from residents reducing their ability to provide compassionate person–centred care which is very essential in management of challenging behaviours. It is therefore unsurprising that settings with high number of abusive episodes produce a lower quality of care environment.
The NSW Nurses Midwives Association (NSWNMA) survey found that over 90% of staff have been subject to some form of aggression from residents.
One of the staff reported, “At residential aged care facility where I work, there is a lot of abuse of staff from residents with cognitive impairment (who cannot be held responsible for such acts legally). They are the one that hit and bite us.”
Another staff reported, “The management tends to take a negative approach when informed by staff, yet publicly they call us to report the cases.”
The number of such staff is increasing.
Increased staff awareness through specialist training programmes within facilities and through peripatetic services can help them cope with these issues. Good care always comes at the cost of appropriate staffing and resources, which are required to ensure that strategies are effective and residents are adequately assessed and supervised.
Abuse of residents
No older person should be subjected to any form of abuse. Elder abuse can be physical, psychological, emotional, sexual or financial. It can be a result of intentional or unintentional neglect.
Dementia or cognitive impairment is a significant and rapidly growing health and social issue in Australia. Majority of the people living with dementia and other form of cognitive impairment are placed in residential aged care facilities. There have been an alarming number of abuses reported every year across Australia. It is said approximately 100,000 abuse cases are reported from throughout Australia per year and many incidents of abuse, neglect and exploitation are not reported. Further, elderly people with cognitive impairment find difficult or impossible to fully comprehend, recall or report the abuse. Even if reported, these reports are sometimes dismissed as unreliable.
Let’s explore some of the residents’ rights in the aged care facility:
- Full and effective use of personal, civil, legal and consumer rights
- Quality care appropriate to needs
- Full information about own state of health and about available treatments
- Treatment with dignity and respect and living without exploitation, abuse or neglect
- Life without discrimination or victimisation and without being obliged to feel grateful to those providing care or accommodation
- Life in safe, secure and homelike environment and free movement both within and outside the facility without undue restriction
- Treatment and acceptance as an individual where their individual preferences taken into account and treated with respect and with privacy
- Continuity of cultural and religious practices and language of own choice
- Selection and maintenance of social and personal relationships with anyone without fear, criticism or restriction
- Maintenance of personal independence and freedom of speech
- Access to services and activities available in the community
- Access to information about rights, care, accommodation and any other information that relates to care recipient
- Access to advocates and other avenues or redress
Let’s think of some of the residents’ responsibilities in the aged care facility:
- Respect the rights and needs of other people within the care facility
- Respect the rights of staff to work in an environment free from harassment
- Care of his or her own health and wellbeing as he or she is capable
- Inform his or her medical practitioner of current health status as he or she is able to
Responsibility of caregivers and nurses
Nursing profession must recognise universal human rights of people and moral responsibility to safeguard the inherent dignity and equal worth of everyone. This includes recognising, respecting and where possible protecting the wide range of civil, cultural, economic, political and social rights that apply to all human beings. The nursing profession acknowledges and accepts the critical relationship between health and human rights and the powerful contribution that human rights can make to improving health outcomes. Accordingly, the profession recognises that accepting the principles and standards of human rights in health care domains involves recognising, respecting, actively promoting and safeguarding the rights of all people/residents to the highest attainable standard of health as fundamental human right.
The Code of Ethics for Nurses has mentioned:
- Nurses value quality nursing care for all people: Valuing quality nursing care involves accepting accountability of the standard of nursing care they provide, helping to raise the standard of nursing care and taking actions when they consider on reasonable grounds.
- Nurses value respect and kindness for self and others: Valuing respect for self and others encompasses valuing the moral worth and dignity of oneself and others.
- Nurses value the diversity of people: Valuing the diversity of people requires nurses to appreciate how different cultural backgrounds and languages may influence both the provision and receipt of nursing and health care.
- Nurses value access to quality nursing and health care for all people: Valuing nursing and health care for all people requires nurses to uphold the principles and standards of the right to nursing and health care as measured by availability, accessibility, acceptability, quality and safety of nursing and health care services.
- Nurses value informed decision making: Nurses value people’s interests in making free and informed decisions.
- Nurses value a culture of safety in nursing and health care: Valuing culture of safety involves nurses actively engaging in the development of shared knowledge and understanding of the crucial importance of safety in contemporary health care.
- Nurses value ethical management of information: The generation and management of information are performed with professionalism and integrity.
- Nurses value a socially, economically and ecologically sustainable environment promoting health and wellbeing: Nurses value strategies at preventing, minimising and overcoming the harmful effects of economic, social or ecological factors on the health of individuals and communities.
On the other hand, reports have said nine of 10 staff suffer abuses. Here are some immediate strategies to help with aggressive behaviour in challenging situations:
Situation 1: Aggressive action or speech: “I don’t want to take a shower!” “I want to go home!” “I don’t want to eat that!”
DOs: Always stay calm, speak in reassuring manner or try and shift the focus to something else.
DON’Ts: Never engage in argument or force the issue that is creating this aggression. Don’t try to forcefully restrain people. The biggest way to stop aggressive behaviour is to remove the word ‘NO’ from a vocabulary.
Situation 2: Confused about place or time: “I want to go home!” “This isn’t my house” “When are we leaving?” “Why are we here?”
DOs: Simple explanations along with photos and other tangible reminders can help. Always say as little as possible about the fact, find another activity, go for a walk, get a snack etc.
DON’Ts: Lengthy explanation or reasons are not the way to go.
Abuse has been a branded silent epidemic since the last decade. Sometimes we hear, listen and see shocking tales of elder abuse. Stories of abuse would make our skin crawl.
The writer is Clinical Specialist working in Australia.




















